The demand for mental and behavioral health services across the United States continues to grow, but reimbursement complexity grows just as fast. Between evolving payer policies, frequent CPT updates, telehealth regulations, and strict documentation standards, billing for mental health providers has become increasingly technical and time-consuming.
For practice owners, therapists, psychiatrists, and behavioral health clinics, the question is no longer whether billing is complicated. The real question is whether outsourcing mental health billing and coding is the right strategic move.
This in-depth guide explains how it works, why practices choose it, and how to select the right partner without risking compliance or revenue.
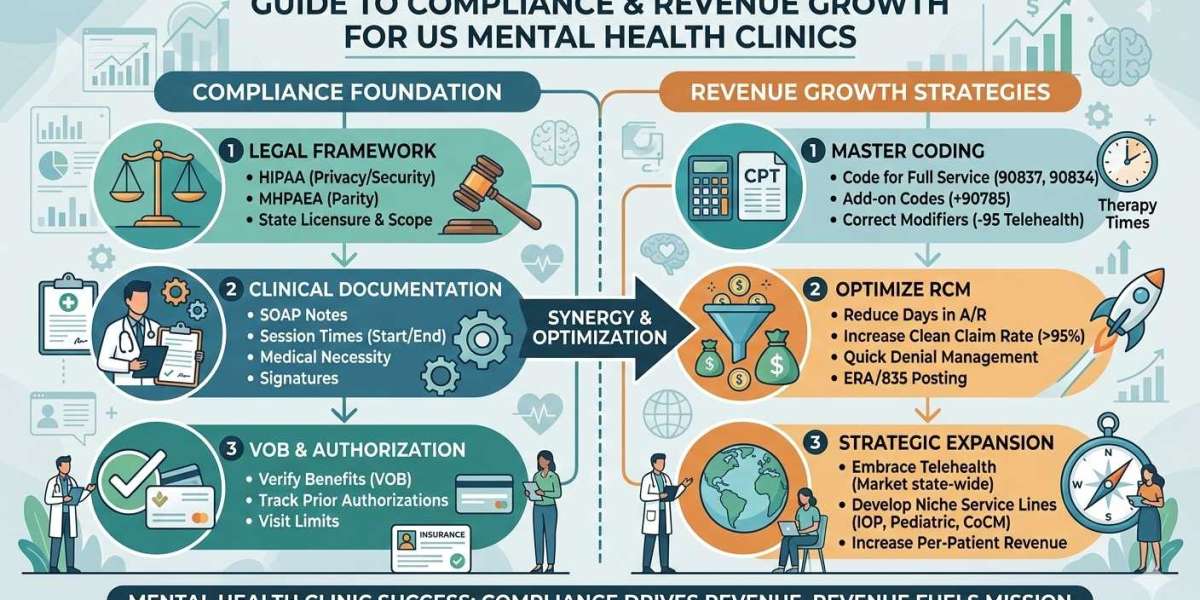
Why Mental Health Billing Is More Complex Than Ever
Mental health medical billing differs from general medical billing in several important ways:
High dependency on accurate documentation for time-based CPT codes
Frequent claim denials due to authorization issues
Strict payer scrutiny on medical necessity
Variations in telehealth billing rules by state
Complex coordination when billing Medicare for mental health services
Coding and billing for mental health services involves psychotherapy codes, medication management, crisis intervention, group therapy, and integrated behavioral health services. Even a small documentation error can lead to denials, delays, or audits.
For solo therapists and group practices, handling billing internally often pulls attention away from patient care.
What Does Outsourcing Mental Health Billing and Coding Mean?
Outsourcing mental health billing and coding refers to partnering with a specialized mental health billing company that manages:
Claims submission
CPT and ICD-10 coding review
Insurance verification
Authorization tracking
Payment posting
Denial management
Accounts receivable follow-up
Compliance monitoring
Instead of hiring in-house staff, practices rely on experienced mental health billing specialist companies that focus solely on revenue cycle tasks.
This approach transforms billing from an administrative burden into a performance-driven process.
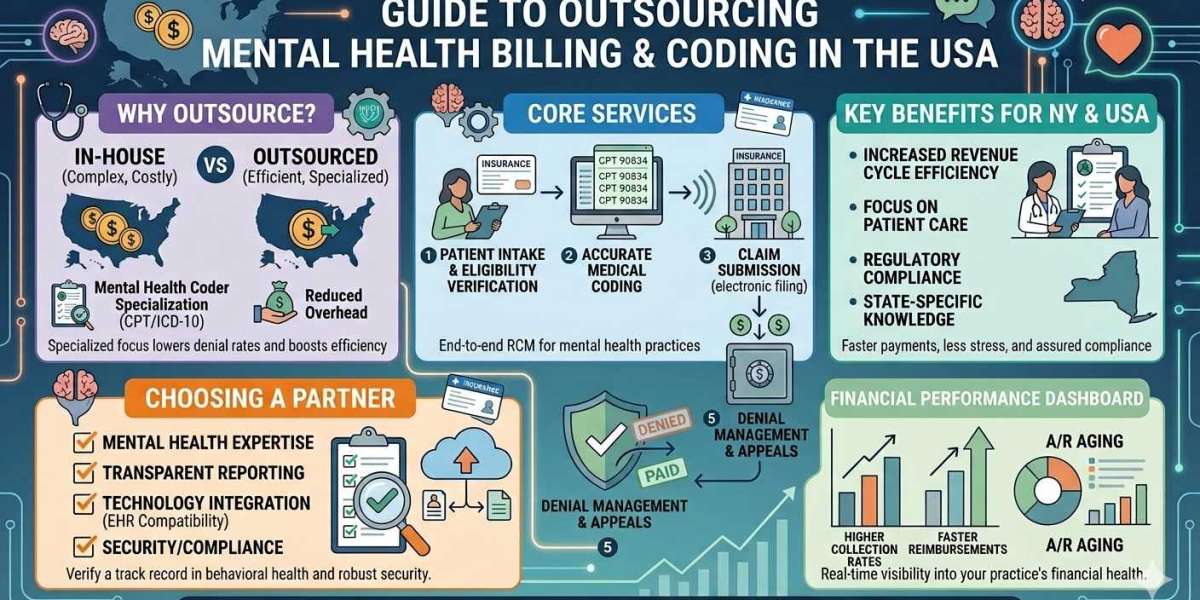
Key Benefits of Outsourced Billing for Mental Health Practices
1. Reduced Claim Denials
Experienced billing companies for mental health understand payer-specific requirements. They monitor trends and prevent recurring errors, improving clean claim rates.
2. Faster Reimbursements
A professional mental health billing services company uses systematic follow-ups and structured workflows to shorten accounts receivable cycles.
3. Regulatory Compliance
Behavioral and mental health billing services must align with HIPAA, Medicare, Medicaid, and commercial payer policies. Outsourced teams stay updated on regulatory changes.
4. Lower Operational Costs
Hiring in-house billers requires salaries, training, benefits, and software investments. Outsourced billing for mental health typically operates on a percentage-based model, reducing fixed overhead.
5. Focus on Patient Care
Therapists and psychiatrists can dedicate more time to clinical outcomes instead of navigating insurance portals.
Who Should Consider Outsourcing?
Outsourcing mental health billing works well for:
Solo therapists struggling with billing Medicare for mental health services
Growing group practices expanding to multiple locations
Behavioral health clinics dealing with high denial rates
Startups needing mental health billing and credentialing services
Providers offering telehealth across state lines
Even established clinics sometimes transition to a top mental health billing company when internal teams face productivity gaps.
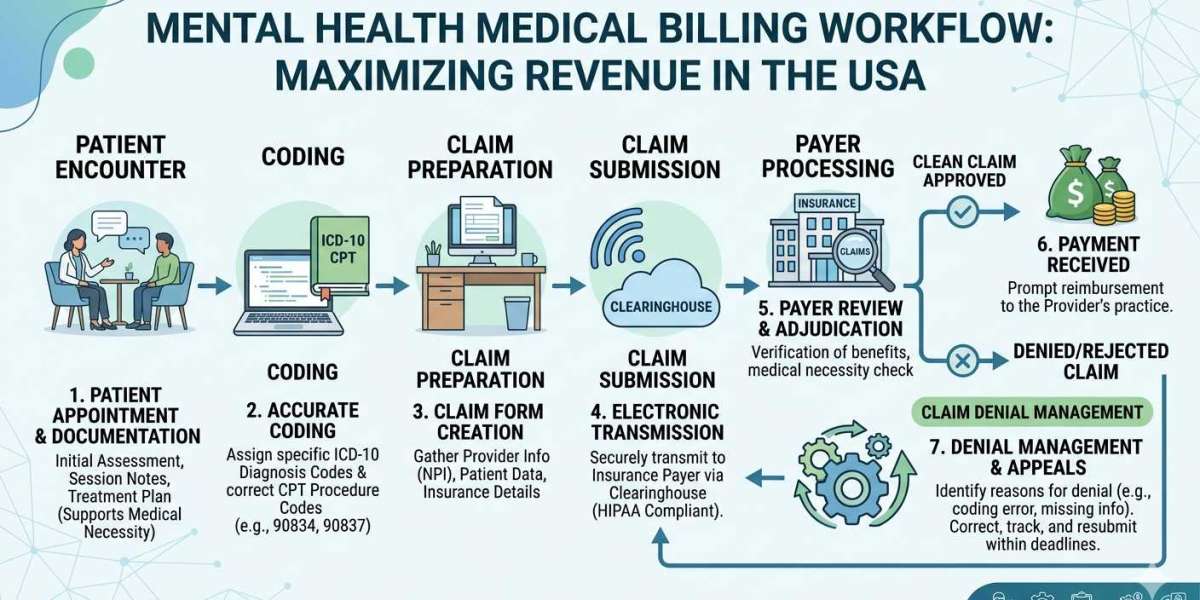
Core Services Provided by a Mental Health Billing Company
A reliable mental health billing solutions provider typically offers:
Insurance Verification and Authorization
Ensuring coverage eligibility before sessions reduces denial risk.
Accurate Coding Review
Medical billing for mental health depends heavily on correct psychotherapy time coding and documentation alignment.
Claims Submission and Tracking
Electronic submission with real-time status monitoring.
Denial Management
Systematic appeals and correction of rejected claims.
Payment Posting and Reporting
Transparent financial reporting improves practice decision-making.
Credentialing Services
Mental health billing and credentialing services help providers enroll with Medicare, Medicaid, and commercial insurers.
How to Choose the Best Mental Health Billing Services Company
Not all vendors are equal. When searching for the best mental health billing company, consider the following:
Industry Specialization
Choose a mental health billing services company that focuses specifically on behavioral health. General billing vendors may lack therapy-specific coding expertise.
Transparent Reporting
Monthly AR reports, denial analysis, and payer performance insights are essential.
Compliance Standards
Verify HIPAA compliance and data security protocols.
Technology Integration
Ensure compatibility with your EHR and practice management software.
Experience with Medicare and Medicaid
Billing Medicare for mental health services requires familiarity with federal documentation standards.
Scalability
A growing clinic should partner with mental health billing specialist companies capable of scaling with expansion.
Addressing the Cost Factor
Many practice owners search for a cheap outsource mental health billing company to reduce expenses. While affordability matters, choosing solely based on low rates can increase long-term revenue loss.
Instead, evaluate value:
Clean claim rate percentage
Average days in AR
Denial recovery success rate
Client retention history
The best outsource mental health billing and coding services balance affordability with performance-driven results.
Common Challenges in Billing for Mental Health Services
Even experienced providers face obstacles:
Time-Based Coding Errors
Psychotherapy codes depend on session length documentation.
Authorization Lapses
Missing prior approvals often leads to denials.
Telehealth Billing Variations
Modifiers and place-of-service codes differ by payer.
Frequent Policy Updates
Insurance policies change frequently in behavioral healthcare.
Professional billing services for mental health clinics proactively track these updates to minimize disruption.
Impact on Revenue Cycle Performance
Effective outsourcing mental health billing directly influences revenue cycle management performance:
Increased clean claim rate
Reduced AR aging
Lower denial ratios
Improved cash flow stability
Enhanced financial forecasting
A structured mental health billing approach creates predictable revenue patterns, which support hiring decisions, service expansion, and marketing investments.
Behavioral and Mental Health Billing Services in 2026
The mental health industry is evolving rapidly:
Teletherapy adoption remains strong
Integrated primary care models are expanding
Value-based care initiatives are increasing
Medicare reimbursement policies are being updated
Billing for mental health therapists now requires ongoing adaptation. Practices that rely on outdated in-house systems often struggle to keep pace.
This is why more providers are shifting toward outsourcing mental health billing as a long-term operational strategy rather than a temporary solution.
The Role of Technology in Mental Health Billing
Modern mental health billing services integrate:
Automated claim scrubbing
Real-time eligibility checks
AI-supported denial pattern analysis
Digital patient statements
Secure cloud-based reporting
Technology enhances human expertise but does not replace it. Skilled billers interpret payer nuances that software alone cannot detect.
When Should a Practice Transition to Outsourcing?
Consider outsourcing if:
Denial rates exceed 10 percent
AR extends beyond 60 days
Staff turnover affects billing consistency
Credentialing delays impact revenue
You plan to expand services or locations
A structured transition plan with a reputable mental health billing company ensures minimal disruption.
Partnering with an Experienced Revenue Cycle Team
A comprehensive provider such as 247 Medical Billing Services offers medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services tailored to behavioral health practices. For clinics seeking reliable billing services for mental health, integrated support across coding accuracy, denial prevention, and credentialing ensures operational stability.
Choosing the right partner means selecting a team that understands billing mental health in detail rather than treating it as a general specialty.
Conclusion
Outsourcing mental health billing and coding is no longer just a cost-saving option. It is a strategic growth decision for practices that want financial clarity, regulatory confidence, and operational efficiency.
With increasing payer scrutiny and complex documentation requirements, working with a specialized mental health billing services company allows providers to focus on patient care while maintaining strong revenue performance. Whether you operate a solo therapy practice or a multi-location behavioral health clinic, outsourced billing for mental health can transform your revenue cycle into a predictable and scalable system.
Frequently Asked Questions
What is outsourcing mental health billing and coding?
It is the process of hiring an external mental health billing company to manage claims submission, coding review, denial management, and revenue cycle tasks for behavioral health providers.
Is outsourcing better than hiring in-house billing staff?
For many practices, yes. Outsourcing reduces overhead costs, improves claim accuracy, and provides access to experienced billing specialists without managing internal payroll and training.
How much does a mental health billing services company charge?
Most billing companies for mental health operate on a percentage of collections model, typically ranging between 4 to 8 percent depending on service scope and practice size.
Can outsourced billing help with Medicare claims?
Yes. Experienced providers handle billing Medicare for mental health services, ensuring compliance with federal documentation and coding standards.
Do billing services include credentialing?
Many mental health billing and credentialing services include payer enrollment, revalidation, and provider credential maintenance.
How long does it take to see improved revenue after outsourcing?
Most practices notice measurable improvements in AR reduction and denial rates within 60 to 90 days after transitioning to professional mental health billing solutions.
Is outsourcing suitable for small therapy practices?
Yes. Billing for mental health therapists can be time-consuming, and outsourcing allows small practices to focus on patient care without administrative burden.