The demand for mental healthcare in the United States has grown rapidly, bringing both opportunity and complexity for providers. While patient care remains the top priority, managing billing processes, insurance claims, and compliance requirements can quickly become overwhelming. This is where billing services for mental health providers play a crucial role in ensuring financial stability and operational efficiency.
Whether you run a private therapy practice or a large behavioral health clinic, understanding how specialized billing solutions work can significantly improve revenue, reduce claim denials, and free up valuable time for patient care.
Why Mental Health Billing Requires Specialized Expertise
Mental health billing is fundamentally different from general medical billing. It involves unique coding systems, varying payer requirements, and strict documentation standards. Providers often deal with psychotherapy session limits, authorization requirements, and frequent policy updates.
A mental health billing specialist understands these complexities and ensures accurate claim submissions. From CPT codes for therapy sessions to ICD-10 diagnosis mapping, every detail must be precise to avoid delays or denials.
Mental health insurance billing services also involve handling pre-authorizations, eligibility checks, and coordination of benefits. Without proper expertise, practices risk losing revenue due to avoidable errors.
Key Benefits of Billing Services for Mental Health Providers
Outsourcing or partnering with a professional billing team offers multiple advantages:
Improved Claim Accuracy
Experts ensure proper coding and documentation, reducing rejection rates.
Faster Reimbursements
Clean claims lead to quicker insurance payments and improved cash flow.
Reduced Administrative Burden
Providers can focus more on patient care instead of paperwork.
Compliance with Regulations
Billing teams stay updated with HIPAA and payer-specific guidelines.
Scalability for Growing Practices
Billing systems adapt as your patient volume increases.
Many practices choose to outsource mental health billing services to streamline operations and maintain consistency in revenue collection.
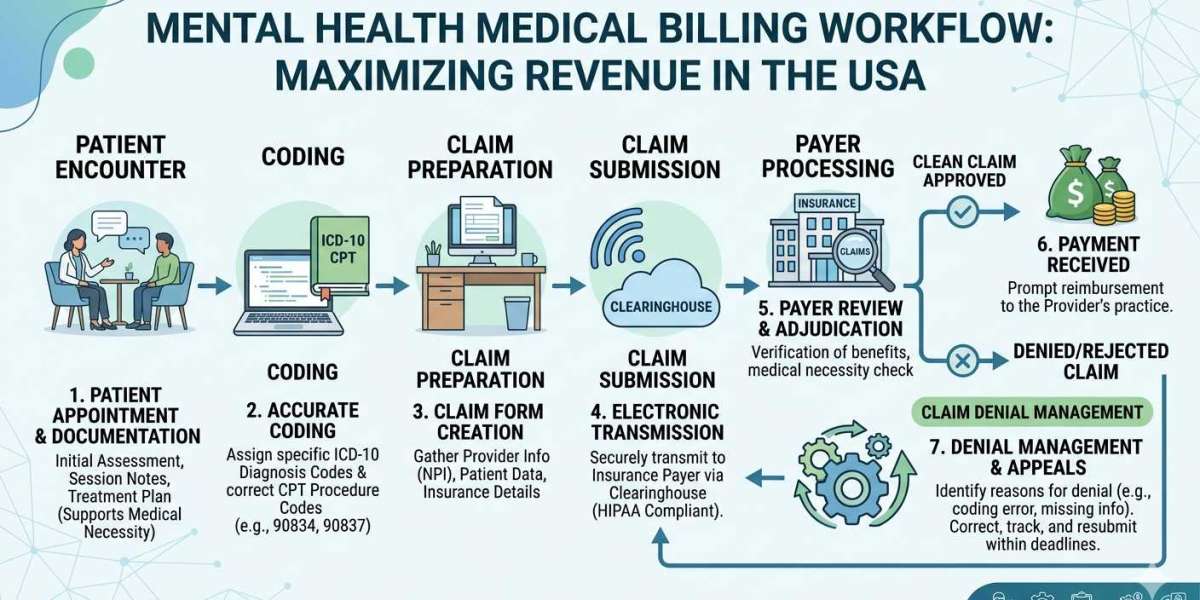
Core Components of Mental Health Billing Services
A reliable mental health billing services agency typically handles end-to-end processes:
Patient Eligibility and Verification
Before appointments, insurance coverage is verified to avoid claim rejections.
Accurate Coding and Documentation
A mental health billing and coding company ensures correct CPT and ICD-10 coding based on therapy type and session duration.
Claim Submission and Tracking
Claims are submitted electronically and tracked for approval status.
Denial Management and Appeals
Denied claims are analyzed and resubmitted with corrections.
Payment Posting and Reporting
Detailed financial reports help providers track revenue and identify trends.
These services collectively form a comprehensive mental health medical billing solution that supports practice growth.
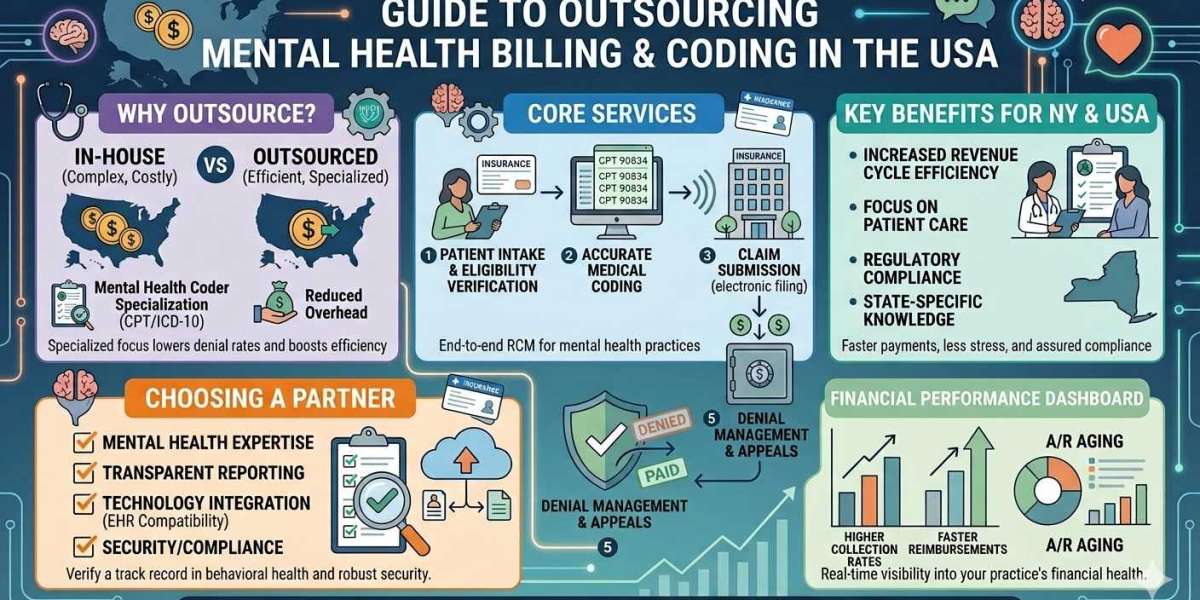
In-House vs Outsourced Mental Health Billing
Many providers struggle with the decision between managing billing internally or choosing outsourced mental health billing.
In-House Billing
Requires hiring and training staff
Higher operational costs
Risk of errors due to limited expertise
Outsourced Billing
Access to experienced professionals
Lower overhead costs
Advanced billing tools and analytics
Outsourced mental health billing often proves more efficient, especially for small to mid-sized practices. Partnering with a top outsource mental health billing company ensures consistent performance and reduced administrative stress.
Choosing the Best Mental Health Billing Agency
Selecting the right partner is critical. Not all mental health billing companies offer the same level of expertise.
Here are key factors to consider:
Industry Experience
Look for a mental health billing provider with proven expertise in behavioral health.
Transparency and Reporting
Regular financial reports and clear communication are essential.
Technology Integration
Ensure compatibility with your EHR or practice management system.
Customization Options
Services should align with your practice size and specialty.
Client Support
Reliable support ensures quick resolution of issues.
The best mental health billing services focus not only on claims processing but also on long-term revenue optimization.
Billing Services for Mental Health Therapists
Independent therapists and small practices face unique challenges. Limited administrative resources often lead to delayed claims and lost revenue.
Billing services for mental health therapists provide tailored solutions, including:
Simplified claim submissions
Automated appointment billing
Insurance follow-ups
Patient billing support
Working with a mental health billing consultant can help therapists identify inefficiencies and improve overall financial performance.
The Role of Technology in Mental Health Billing
Modern mental health medical billing services rely heavily on technology to improve efficiency and accuracy.
Key innovations include:
Automated Claim Scrubbing
Identifies errors before submission
Real-Time Eligibility Checks
Reduces claim denials
Analytics and Reporting Tools
Provides insights into revenue trends
Cloud-Based Systems
Enables secure access and scalability
A strong mental health medical billing services outsourcing partner leverages these technologies to deliver consistent results.
Common Challenges in Mental Health Insurance Billing
Even experienced providers face recurring challenges:
Frequent policy changes by insurance companies
Complex authorization requirements
High denial rates for psychotherapy claims
Time-consuming follow-ups
Mental health insurance billing becomes manageable when handled by a professional mental health billing agency that understands payer-specific nuances.
How a Professional Mental Health Billing Company Improves Revenue
A professional mental health billing company goes beyond basic claim processing. It actively identifies revenue gaps and implements strategies to maximize collections.
This includes:
Identifying underpaid claims
Reducing days in accounts receivable
Improving first-pass claim acceptance rates
Ensuring compliance with evolving regulations
By partnering with the best outsource mental health billing and coding company, providers can achieve sustainable financial growth.
Behavioral Mental Health Billing Services for Group Practices
Group practices and clinics require more advanced billing solutions due to higher patient volumes and multiple providers.
Behavioral mental health billing services support:
Multi-provider scheduling and billing
Centralized reporting systems
Coordination across different insurance plans
Streamlined revenue cycle processes
A dedicated mental health billing companies team ensures smooth operations across all departments.
Future Trends in Mental Health Billing
The landscape of mental health billing continues to evolve with changes in healthcare policies and technology.
Key trends include:
Increased adoption of telehealth billing
Value-based care reimbursement models
Integration of AI-driven billing tools
Enhanced patient payment solutions
Providers who adapt to these changes with the help of a mental health billing specialist will stay ahead in a competitive market.
Conclusion
Billing services for mental health providers are no longer optional; they are essential for maintaining financial health and operational efficiency. With increasing complexities in insurance policies and coding requirements, relying on expert billing solutions ensures accuracy, compliance, and steady revenue growth.
Whether you choose a mental health billing agency, a mental health billing consultant, or a full-scale mental health medical billing solution, the right partner can transform your practice. From reducing administrative burden to improving claim success rates, professional billing services empower providers to focus on what matters most—delivering quality mental healthcare.
For practices seeking comprehensive support, integrating services such as medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services ensures a complete and seamless operational framework. Companies like 247 medical billing services offer integrated solutions tailored to the evolving needs of mental health providers.
FAQs
What are billing services for mental health providers?
Billing services for mental health providers handle insurance claims, coding, payment processing, and revenue management specifically for behavioral health practices.
Why should I outsource mental health billing services?
Outsourcing reduces administrative workload, improves claim accuracy, and ensures faster reimbursements through expert handling.
How does a mental health billing specialist help my practice?
A specialist ensures proper coding, manages claims efficiently, and minimizes denials, leading to improved revenue.
What is included in mental health insurance billing services?
These services include eligibility verification, claim submission, denial management, and payment tracking.
How do I choose the best mental health billing agency?
Look for experience, transparency, advanced technology, and strong client support when selecting a billing partner.
Are billing services for mental health therapists different from large practices?
Yes, they are often customized to suit smaller operations, focusing on simplicity and cost-effectiveness.
What is the benefit of outsourced mental health billing?
It provides access to experienced professionals, reduces costs, and improves overall billing efficiency.
Can a mental health billing consultant improve revenue?
Yes, consultants analyze existing processes, identify inefficiencies, and recommend strategies to maximize collections.