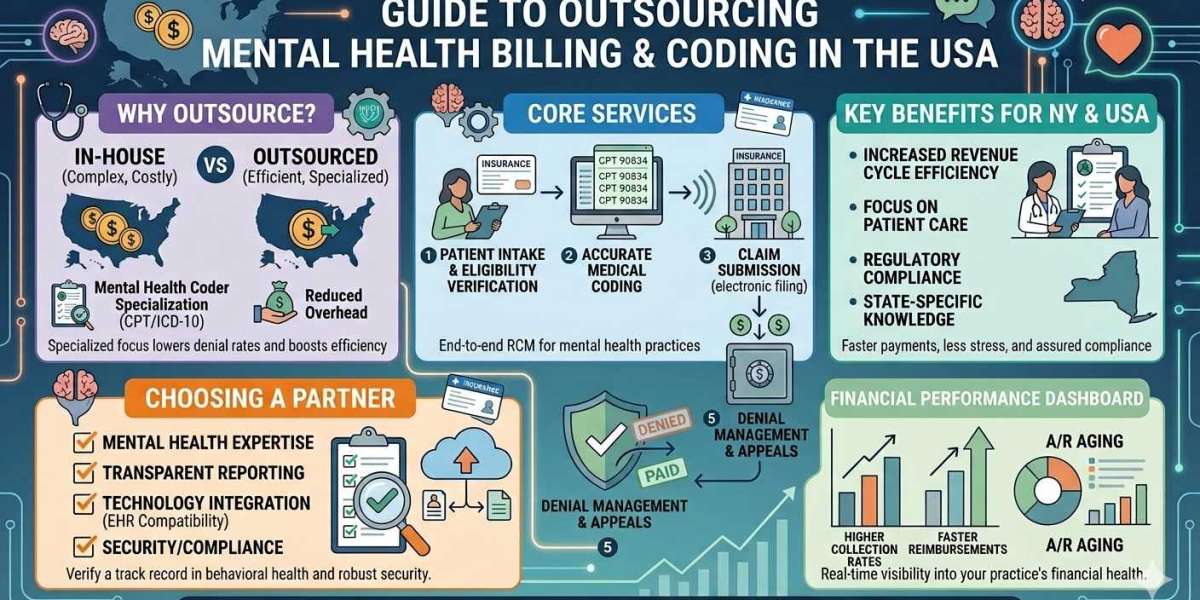
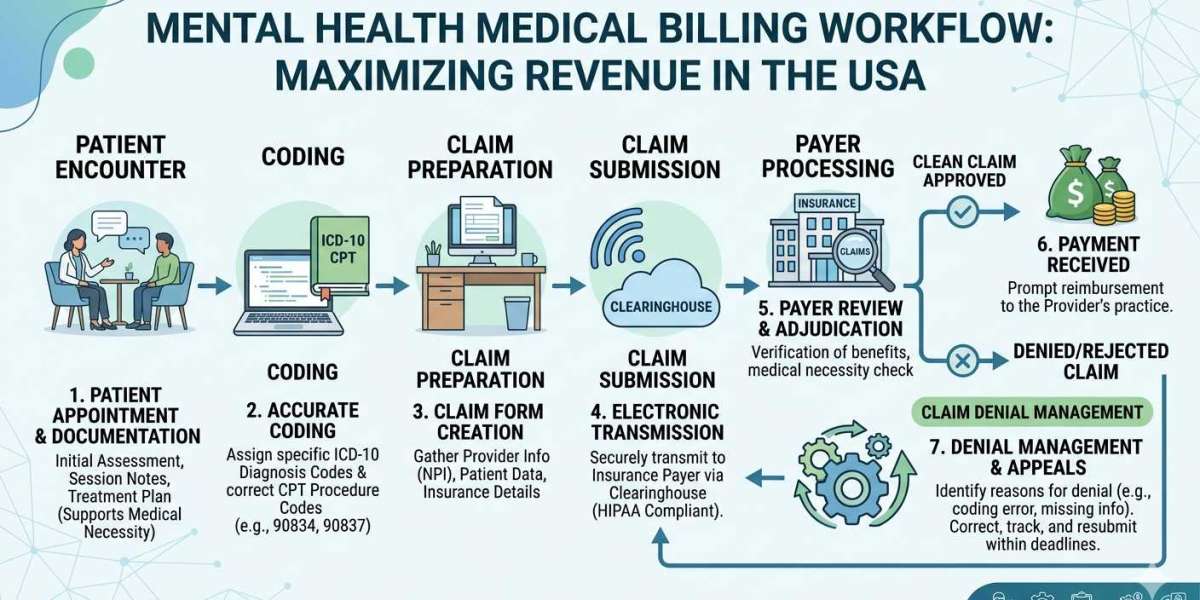
The behavioral health sector is growing rapidly, but with that growth comes increasing administrative complexity. Providers in Connecticut are facing challenges such as evolving payer policies, strict compliance requirements, and rising claim denials. This is where behavioral health billing services Connecticut play a crucial role in ensuring financial stability and operational efficiency.
Whether you run a private practice, a community mental health center, or a multi-specialty behavioral clinic, having an optimized billing process directly impacts your revenue cycle. This blog explores everything you need to know about behavioral health billing, why outsourcing is becoming essential, and how providers can improve collections while reducing administrative burden.
Understanding Behavioral Health Billing in Connecticut
Behavioral health billing differs significantly from general medical billing. It involves unique coding structures, session-based billing, time-based CPT codes, and strict documentation requirements. Services such as psychotherapy, substance abuse treatment, and psychiatric evaluations require precision in coding and claim submission.
In Connecticut, insurance regulations and payer guidelines can vary widely, making it essential for providers to stay updated. Even small errors in documentation or coding can lead to delays, denials, or compliance risks.
That’s why many providers are turning to professional behavioral health billing company Connecticut solutions to manage their revenue cycle more effectively.
Key Challenges Faced by Behavioral Health Providers
Behavioral health practices often struggle with:
Complex CPT and ICD coding requirements for therapy sessions
Frequent claim denials due to documentation gaps
Delayed reimbursements affecting cash flow
Prior authorization requirements for certain treatments
Managing multi-payer systems with different policies
Compliance with state and federal regulations
These challenges make it difficult for providers to focus on patient care, pushing them to consider outsourcing behavioral health billing services Connecticut for better efficiency.
Why Outsourcing Behavioral Health Billing is a Smart Choice
Outsourcing has become a strategic move for behavioral health providers across the United States. From outsourcing behavioral health billing ohio to outsourcing behavioral health billing texas, practices are recognizing the value of specialized billing partners.
When you outsource, you gain access to:
Experienced billing professionals
Advanced billing software and automation
Reduced administrative workload
Faster claim submissions and reimbursements
Improved compliance and audit readiness
For providers in Connecticut, outsourcing behavioral health billing services connecticut ensures that local payer rules and compliance standards are handled with precision.
How Behavioral Health Billing Services Improve Revenue Cycle
A well-managed billing system directly impacts your revenue cycle management. Here’s how professional services help:
Accurate Coding and Documentation
Specialized billing teams ensure correct CPT and ICD coding, reducing claim rejections.
Faster Claims Processing
Electronic claim submission speeds up reimbursements and minimizes delays.
Denial Management
Dedicated teams analyze and resolve denied claims, improving recovery rates.
Eligibility Verification
Pre-verification ensures patients are covered, reducing unpaid claims.
Compliance Assurance
Billing experts stay updated with regulations, protecting practices from audits.
Providers using behavioral health billing services north carolina or behavioral health billing services rhode island have reported similar improvements, showing how scalable these solutions are across states.
The Growing Demand Across the U.S.
Behavioral health billing services are not limited to Connecticut. Across the country, practices are leveraging outsourcing solutions to stay competitive.
For example:
behavioral health billing company california providers are adopting automation to handle high patient volumes
outsourcing behavioral health billing virginia is helping clinics manage Medicaid and private payer complexities
behavioral health billing company georgia practices are focusing on reducing AR backlogs
behavioral health medical billing utah providers are improving compliance with state-specific regulations
Even in smaller markets, such as behavioral health billing columbus ohio or behavioral health billing ohio, outsourcing is becoming a standard practice for growth-oriented clinics.
Community Behavioral Health and Billing Needs
Community health organizations have unique billing challenges due to diverse patient populations and funding sources. Programs often include Medicaid, grants, and sliding fee structures.
Solutions like outsourcing community behavioral health billing ohio or community behavioral health billing services company delaware help organizations manage:
Complex funding structures
Government program compliance
High patient volumes with limited staff
Reporting requirements for grants and audits
These services ensure that community providers remain financially sustainable while serving vulnerable populations.
Choosing the Right Behavioral Health Billing Partner
Selecting the right billing company is critical for long-term success. Here are key factors to consider:
Experience in Behavioral Health
Choose a company with proven expertise in mental health and substance abuse billing.
Technology and Automation
Advanced billing software improves accuracy and reduces turnaround time.
Transparency and Reporting
Regular reports on claims, denials, and collections provide better financial visibility.
Compliance Knowledge
Ensure the partner understands HIPAA, payer rules, and state regulations.
Scalability
Your billing partner should grow with your practice.
Whether you are considering a professional behavioral health billing company new hampshire or a top behavioral health billing company virginia, the focus should always be on expertise and reliability.
Multi-State Billing Expertise Matters
Many providers operate in multiple states or plan to expand. In such cases, working with a billing partner experienced across regions is essential.
For instance:
outsourcing behavioral health billing services florida helps manage diverse payer networks
outsourcing behavioral health medical billing services provider in florida ensures compliance with state-specific policies
best behavioral health billing company south carolina offers tailored solutions for regional practices
professional behavioral health billing company rhode island focuses on smaller practice optimization
A multi-state billing approach ensures consistency in revenue management while adapting to local regulations.
Technology’s Role in Modern Behavioral Health Billing
Technology is transforming the billing landscape. From AI-driven claim analysis to automated eligibility checks, modern tools are improving efficiency.
Key innovations include:
Automated coding assistance
Real-time claim tracking
Integrated EHR and billing systems
Data analytics for revenue optimization
These tools are widely used by behavioral health billing services in california and other advanced markets, setting a benchmark for providers nationwide.
Why Connecticut Providers Need Specialized Billing Services
Connecticut has a unique healthcare landscape with a mix of private insurance, Medicaid programs, and strict compliance requirements.
Behavioral health billing services connecticut are tailored to address:
State-specific Medicaid guidelines
Insurance verification complexities
High documentation standards
Audit preparedness
By working with a professional behavioral health billing company connecticut, providers can focus more on patient care while ensuring financial stability.
Future Trends in Behavioral Health Billing
The future of behavioral health billing is driven by:
Increased adoption of telehealth billing
Value-based care models
Automation and AI integration
Enhanced data security measures
Practices that adapt to these trends will be better positioned for long-term growth and sustainability.
Conclusion
Behavioral health billing is no longer just an administrative task—it is a critical component of a practice’s financial health. With increasing complexities in payer requirements and compliance standards, providers must adopt smarter billing strategies.
Behavioral health billing services connecticut offer a reliable solution to streamline operations, reduce denials, and improve revenue cycles. Whether you are a small practice or a large behavioral health organization, outsourcing can provide the expertise and efficiency needed to thrive.
Partnering with an experienced provider like 247 medical billing services ensures access to comprehensive solutions including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services, all designed to support sustainable growth and operational excellence.
FAQs
What are behavioral health billing services?
Behavioral health billing services handle coding, claim submission, and reimbursement processes for mental health and substance abuse treatment providers.
Why is behavioral health billing complex?
It involves time-based coding, strict documentation requirements, and varying payer rules, making accuracy essential.
How can outsourcing improve revenue?
Outsourcing reduces errors, speeds up claim processing, and improves denial management, leading to higher collections.
Is outsourcing suitable for small practices?
Yes, even small practices benefit from reduced administrative workload and improved cash flow.
What should I look for in a billing company?
Experience in behavioral health, compliance knowledge, advanced technology, and transparent reporting are key factors.
Are these services only for Connecticut providers?
No, similar solutions are available nationwide, including behavioral health billing services north carolina, behavioral health billing services rhode island, and behavioral health billing company california.
How does technology help in billing?
Technology automates processes, reduces errors, and provides real-time insights into revenue performance.