When considering any dermatological procedure, understanding the clinical boundaries of safety and the biological timeline of healing is paramount. Mole Removal in Dubai has reached a gold standard in 2026, utilizing non-invasive diagnostic tools and high-precision extraction methods that prioritize patient well-being. By focusing on evidence-based safety protocols, medical professionals can offer results that are both aesthetically pleasing and medically sound, ensuring that every patient feels secure throughout their transformation.
The Clinical Framework of Mole Removal in Dubai
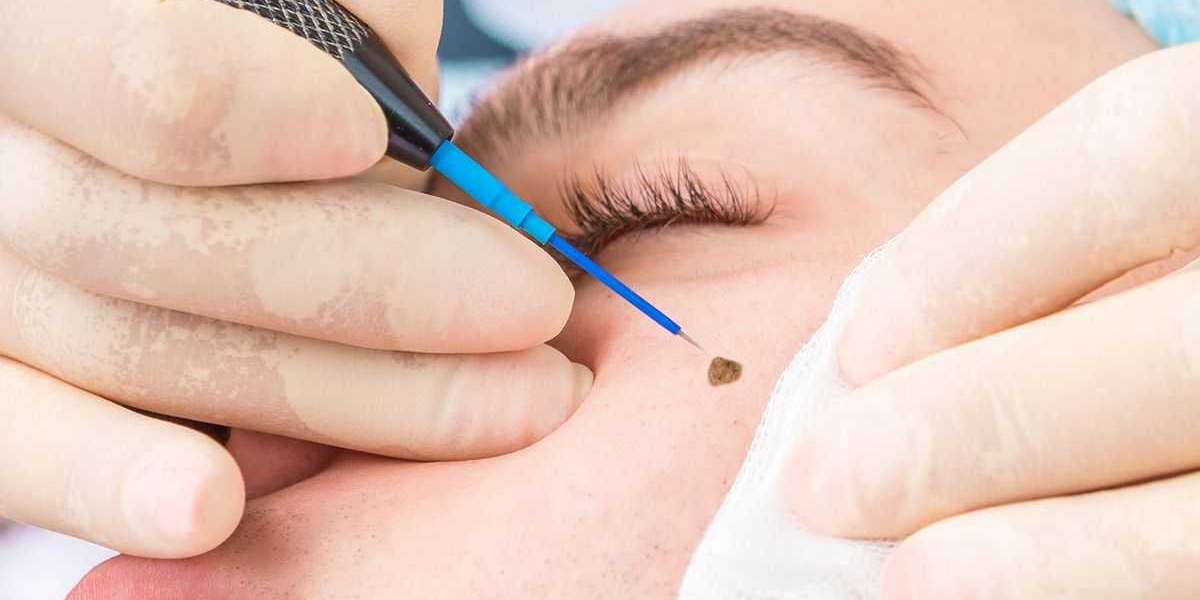
Safety in dermatology begins with an expert "differential diagnosis." Before any lesion is treated, it must be categorized as benign, atypical, or suspicious. In our clinical experience, the use of digital dermoscopy—a high-magnification imaging technique—is the first line of defense. This allows for the visualization of pigment patterns that are invisible to the naked eye.
Choosing Mole Removal in Dubai means your procedure is conducted within a regulated medical environment that adheres to strict sterilization and procedural standards. This clinical framework is designed to eliminate the risks associated with "do-it-yourself" or non-medical treatments, which often lead to deep-seated infections or permanent scarring. What patients typically report during recovery is that the peace of mind provided by a professional setting is just as valuable as the physical result itself.
The Mechanism: Hemostasis and Tissue Preservation
The mechanism of modern removal focuses on "controlled trauma." Whether using a CO2 laser or a surgical shave, the goal is to remove the target tissue while instantly sealing the surrounding area. Laser technology achieves this through thermal coagulation, which closes blood vessels as the mole is vaporized.
For surgical methods, the mechanism involves a precise tangential excision. This allows the specialist to remove the mole flush with the skin surface without damaging the deeper dermal layers. In our clinical experience, the "depth-control" afforded by 2026 surgical tools is what prevents the sunken or "pitted" appearance often seen in older extraction techniques. By preserving the underlying skin architecture, we ensure the body can heal across a flat, stable surface.
The Purpose: Health Surveillance and Comfort
The primary purpose of professional removal is the mitigation of future skin risks. In a high-UV climate, moles are dynamic; they can change in response to sun damage over time. Removing an atypical mole serves the purpose of "interruption," stopping a potentially problematic growth before it can evolve further.
Additionally, the purpose is often functional. Moles that reside in areas of constant friction, such as the neck, underarms, or groin, are subject to repeated micro-trauma. This can cause the mole to become chronically inflamed or tender. Professional extraction provides a permanent solution to this physical annoyance, allowing patients to move and dress without the constant worry of irritation or bleeding.
Benefits of a Safety-First Approach
Infection Control: Procedures are performed in a sterile surgical suite.
Minimized Scarring: Advanced energy tools promote regenerative healing over scar formation.
Histological Accuracy: The ability to send tissue for biopsy ensures 100% medical certainty.
Zero Pain: Modern local anesthetics provide complete numbness during the procedure.
| Safety Feature | Clinical Benefit |
| Dermoscopy | Accurate pre-surgical screening. |
| Cold-Laser Tech | Reduces thermal damage to healthy skin. |
| Medical Barrier | Protects the wound from Dubai's environmental dust. |
Ideal Candidates for Safe Extraction
Ideal candidates are individuals with benign or atypical moles who are in good overall health. We prioritize patients who understand the importance of post-operative care, particularly the need for strict sun avoidance during the initial healing phase. During the consultation, we also screen for any history of keloid scarring or pigment disorders. This ensures that the chosen removal method is perfectly calibrated to the patient's specific skin biology, maximizing both safety and aesthetic success.
The Procedural Steps: Ensuring a Safe Outcome
Dermatoscopic Mapping: Identifying the mole's "safe zones" for extraction.
Antiseptic Preparation: Thoroughly cleansing the area to prevent bacterial entry.
Anesthetic Injection: Administering a local numbing agent to ensure zero discomfort.
Precision Removal: Using the selected modality (Laser, RF, or Shave) to extract the mole.
Biopsy Submission: Securing the specimen in a sterile container if analysis is required.
Protective Sealing: Applying a clinical-grade antibiotic and a specialized bandage.
Common Areas for Treatment and Safety Considerations
Safety protocols are adapted based on the anatomical location of the mole:
The Eyelids and Periorbital Area: Requires the use of specialized ocular shields.
The Hands and Feet: Areas with less "slack" skin that require tension-free removal.
The Scalp: Careful management of hair follicles to ensure no permanent hair loss at the site.
The Back: Monitoring for high-tension healing that might lead to wider scars.
Cost and Complexity Factors in Modern Care
The factors influencing the procedural process include the size of the lesion and the necessity of laboratory pathology. A simple laser vaporization of a small, benign facial mole is a straightforward clinical event. However, a large, multi-colored mole requiring deep excision and lab analysis involves more resources and time. In our clinical experience, the value of the procedure is reflected in the expertise of the medical team and the high-end technology used to ensure a "one-and-done" result.
The Recovery Timeline: Stages of Regeneration
The Inflammatory Phase (Days 1–3): Mild redness and swelling as the body sends repair cells to the site.
The Proliferative Phase (Days 4–14): A thin, flat scab forms and eventually falls off, revealing pink "new skin."
The Remodeling Phase (Month 1–6): The skin gains strength and the color fades to match the surrounding area.
What patients typically report during recovery is that the site feels "tight" or slightly itchy during week two; this is a positive sign that the nerves and collagen fibers are successfully reconnecting.
Potential Side Effects and Safety Guardrails
Even with the best technology, the body has a natural response to treatment. Temporary side effects may include localized bruising or "post-inflammatory hyperpigmentation" (PIH), where the skin temporarily darkens. To ensure safety, we provide every patient with a specialized "rescue cream" to manage these responses. We also strictly advise against swimming or heavy sweating for the first 48 hours to prevent the wound from becoming macerated or exposed to bacteria.
Post-Treatment Maintenance for a Perfect Result
The final safety step is long-term protection. The new skin is "naive" and lacks the melanin protection of the surrounding tissue. We emphasize the daily application of a broad-spectrum SPF 50, even if the patient is spending most of their day indoors. Utilizing silicone-based scar gels starting in week three can also help ensure the site remains flat and soft, preventing any textural irregularities from developing over time.
Conclusion
Choosing a professional path for skin refinement ensures that your journey is as safe as it is transformative. By prioritizing medical standards and following a structured recovery plan, you can achieve a clear complexion without compromising the health of your skin. Reclaiming your confidence is a seamless process when guided by expertise and advanced clinical technology. Learn if this treatment is right for your lifestyle by booking a consultation at Tajmeels Clinic.